Obamacare’s Impact On Healthcare Spending: 3 Charts That Show Why The Newly Insured Are More Expensive
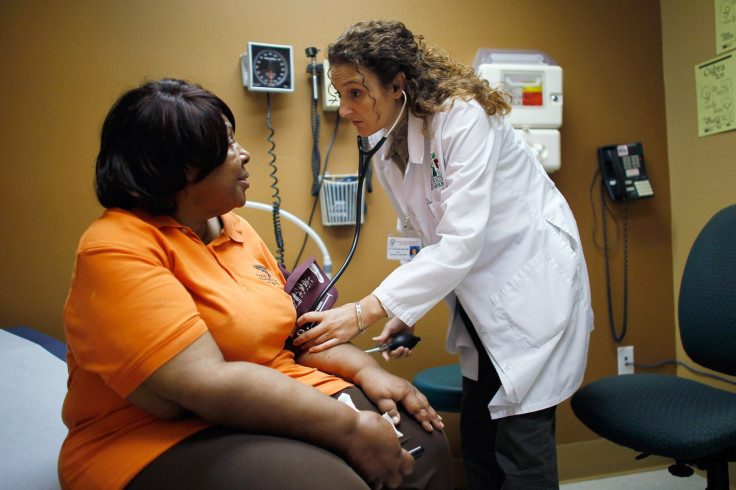
In the six years since the Affordable Care Act became law, critics of the administration's most prized domestic policy have warned unceasingly of a resultant "death spiral." Only the sickest, most expensive patients would sign up for health insurance on individual exchanges, they predicted. Now, a report released Wednesday from the Blue Cross and Blue Shield Association suggests those naysayers were right, in a limited sort of way. Here are four key takeaways from the report.
1. Patients who signed up for health insurance on individual exchanges created by the Affordable Care Act were indeed sicker, the report shows. The Blue Cross and Blue Association is the dominant health insurer on those exchanges, and based its findings on a study of its 4.7 million policyholders.
Just how much sicker were the new Obamacare enrollees, compared to their peers? As the chart below shows, they had higher prevalence of diabetes, depression and heart disease than other pools of enrollees. Only with hypertension were those covered by employer-based insurance sicker, but only slightly.
2. Because the costs of doctor visits and drugs add up, those sicker patients are more expensive. In 2015, medical costs associated with the new enrollees were 22 percent higher than those with employer-based coverage, with an average of $559 in monthly medical spending compared to $457.
Why? With higher rates of diseases and conditions, like the ones cited above, people who enrolled prior to 2014, or were covered through their employers, went to the doctor or the hospital more frequently, had more prescriptions filled and visited emergency rooms more, the report found.
Here's a rough breakdown of the patients who used those medical services, and how often:
3. The Obama administration says this report shows why Obamacare was necessary in the first place. “It’s no surprise that people who newly gained access to coverage under the Affordable Care Act needed health care,” Ben Wakana, a spokesman for the Department of Health and Human Services, told the New York Times. “That’s why they were locked out of coverage before.”
Prior to the Affordable Care Act, insurers were able to deny coverage to patients with pre-existing conditions. So if a person had an illness or a health problem, be it asthma or cancer, when they went to buy health insurance, insurers could deny them coverage or charge them more.
The Affordable Care Act more or less banned that practice. As a result, when the law went into effect, the health insurance market was flooded with many patients who had pre-existing conditions that may not have been treated or managed, sometimes for years.
4. These numbers don't necessarily spell doom for healthcare in America, or mean that death spirals are inevitable — as long as everyone pitches in. "The findings underscore the need for all of us in the healthcare system, and newly insured consumers, to work together to make sure that people get the right healthcare service in the right care setting and at the right time," Alissa Fox, senior vice president of the office of policy and representation for the Blue Cross Blue Shield Association, said in a press release.
In the medical world (among others), an ounce of the right prevention is worth at least a pound of cure. Everyone, from tech startups to health insurers, is experimenting with and pioneering ways to help people become healthier — to entice them to exercise more by offering monetary rewards, for example — and prevent illness. The aim, of course, is to reduce healthcare costs as well.
While the jury is still out on which kinds of programs are most effective, if successful programs are widely implemented, they could help reduce healthcare spending. And, of course, as more people gain insurance, including those with pre-existing conditions, they ideally gain access to doctors and medicines that help catch and treat illnesses before they reach more advanced — and more expensive — stages.
© Copyright IBTimes 2024. All rights reserved.






















